In the modern surgical suite, the hazards of surgical smoke—plumes generated by lasers, electrosurgical units (ESU), and ultrasonic devices—are well-documented. Containing over 150 hazardous chemicals and viable biological particulates, this “byproduct” is a significant occupational health risk for dermatologists, nurses, and technicians.
To mitigate this risk, smoke evacuators are mandatory. However, not all filtration systems are created equal. While HEPA (High-Efficiency Particulate Air) filters have long been the industry standard, ULPA (Ultra-Low Penetration Air) filters represent a critical evolution in protection.
At Acuderm, our Evac systems utilize ULPA technology. Here is a technical breakdown of why ULPA filtration—specifically those rated at 99.99997% efficiency—is the superior choice for your practice.
The Fundamental Difference: HEPA vs. ULPA
The distinction between HEPA and ULPA lies in the “tightness” of the filter media and the size of the particles they are validated to capture.
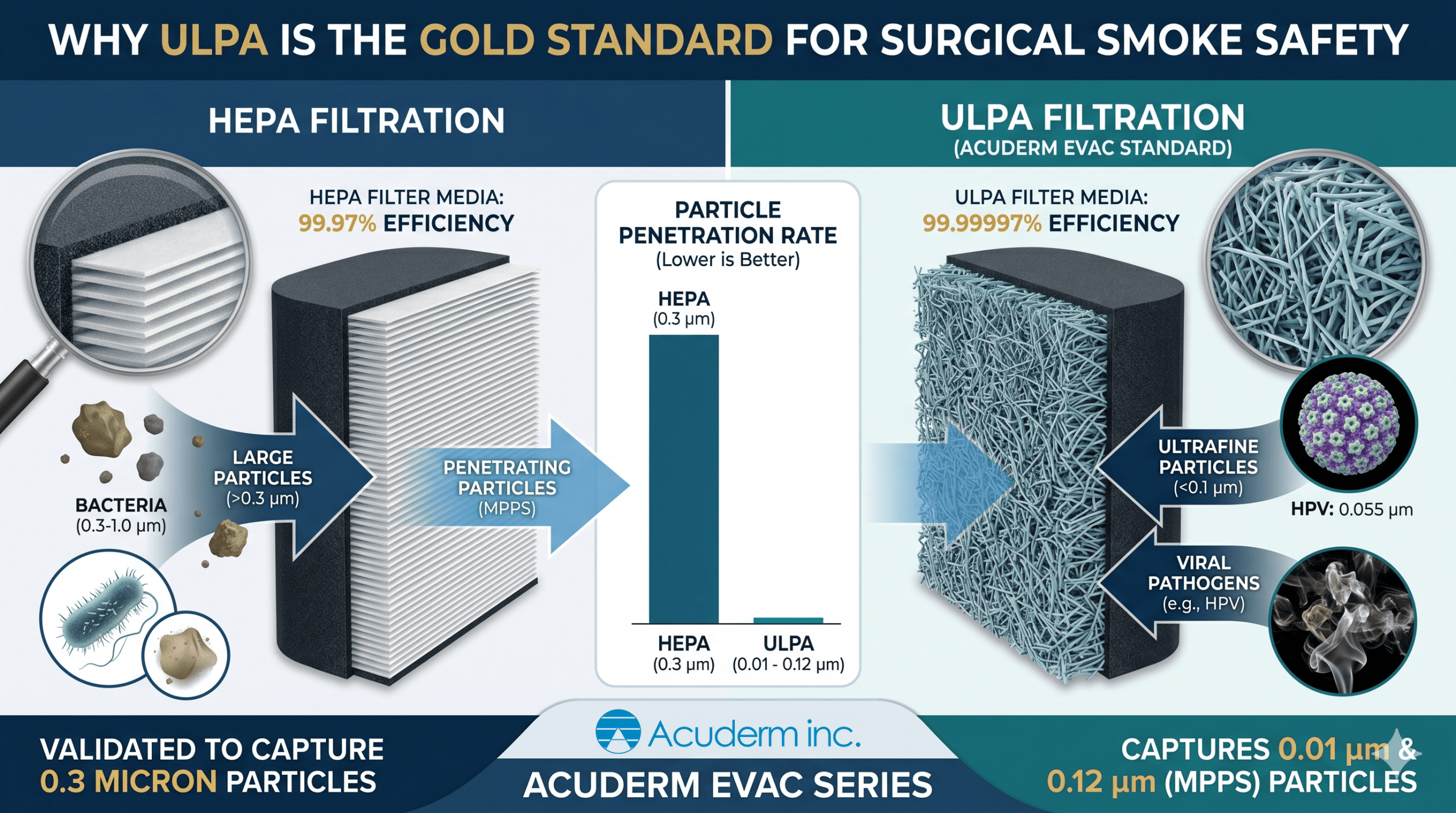
- HEPA Filters: Typically rated to capture 99.97% of particles at 0.3 microns.
- ULPA Filters: Rated to capture 99.999% or higher of particles at 0.1 to 0.12 microns.
Acuderm’s ULPA filters push this even further, achieving 99.99997% efficiency on particles as small as 0.01 micron and at the Most Penetrating Particle Size (MPPS) of 0.12 microns.
Understanding the MPPS Gap
A common misconception in filtration is that smaller particles are always harder to catch. In reality, particles around 0.1 to 0.3 microns are the most difficult to trap because they are too large to be easily moved by Brownian motion (diffusion) but too small to be easily caught by mechanical interception. This range is known as the Most Penetrating Particle Size (MPPS).
While a HEPA filter’s efficiency begins to drop significantly as particles approach the 0.1-micron mark, an ULPA filter is specifically engineered to maintain peak efficiency at this critical threshold.
Why the 0.01 to 0.12 Micron Range Matters
In dermatology and laser surgery, the “targets” we aim to capture are often much smaller than the 0.3-micron HEPA benchmark.
- Viral Pathogens: The Human Papillomavirus (HPV), frequently aerosolized during the treatment of verrucae or condyloma, measures approximately 0.055 microns. A HEPA filter is not validated to capture particles of this size with the same rigor as an ULPA filter.
- Ultrafine Particles (UFPs): Laser plumes produce a high concentration of ultrafine particles (less than 0.1 microns). These particles can bypass the upper respiratory tract and settle deep within the alveoli of the lungs, potentially entering the bloodstream.
- DNA Fragments: Research has shown that intact viral DNA can be recovered from laser plumes. ULPA filters provide the necessary density to ensure these fragments are sequestered within the filter media.
Quantifying the Efficiency: The Math of Safety
The difference between 99.97% (HEPA) and 99.99997% (Acuderm ULPA) may seem negligible, but from a clinical safety perspective, it is a massive leap:
- HEPA (99.97%): Allows 300 out of every 1,000,000 particles to pass through.
- Acuderm ULPA (99.99997%): Allows only 3 out of every 10,000,000 particles to pass through.
In a high-volume dermatology clinic where laser procedures are performed daily, that 1,000-fold increase in protection significantly reduces the cumulative exposure for the surgical team.
Clinical Implications for the Surgical Team
For the laser technician and the circulating nurse, the use of an ULPA-rated evacuator like the Acuderm Evac means:
- Superior Odor Control: ULPA filters are often paired with advanced charcoal filtration to neutralize Volatile Organic Compounds (VOCs) and benzene.
- Reduced Cross-Contamination: By capturing particulates at the 0.01-micron level, the risk of viable biological material remaining in the room air is virtually eliminated.
Conclusion
In the hierarchy of personal protective equipment, the filter is the heart of the system. While HEPA is suitable for general air purification, the specialized environment of a laser or electrosurgical suite demands the precision of ULPA.
By choosing a system rated at 99.99997% efficiency at 0.12 microns, you aren’t just following a protocol—you are implementing the highest possible standard of respiratory protection for yourself, your staff, and your patients.
Explore the technical specifications of the Acuderm Evac series here.
Sources:
- NIOSH (National Institute for Occupational Safety and Health) – Research on Surgical Smoke Hazards.
- ANSI/AAMI ST108:2023 – Water for the processing of medical devices (Principles for air quality and filtration).
- Journal of the American Academy of Dermatology (JAAD) – Studies on HPV DNA in laser plumes.
